Rib grafting for Maxillofacial procedures
A graft is any living tissue that can be transplanted surgically from the donor site to the recipient site. When this tissue is obtained from the same patient for whom rib grafting is required, it is known as an autograft. Many maxillofacial procedures require grafts for replacement of the lost tissue. Out of the many autograft options available, the costochondral graft (rib graft) is one of the i.deal options for maxillofacial procedures. The advantage of this graft is that it can provide either bone or cartilage or both and bone & cartilage. They are harvested depending on patient needs.
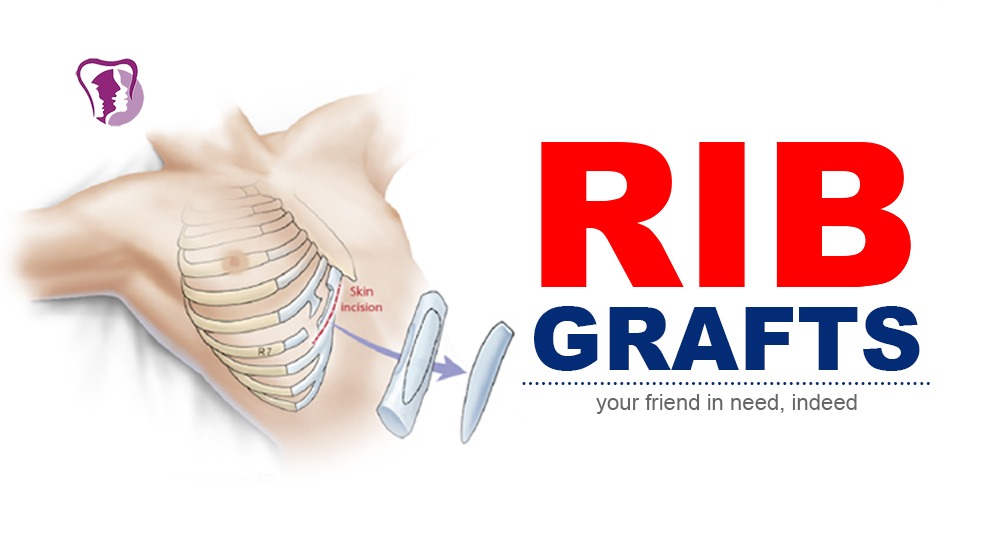
The rib grafting can be used for maxillofacial procedures like TMJ ankylosis, reconstruction of the nasal bridge, reconstruction of orbital floor in trauma cases, interposition graft in corrective jaw surgeries, only graft for sunken jaws, reconstruction of an ear, and coverage of brain when a part of the skull bone has been lost. When the rib bone graft along with cartilage is used in cases of TMJ ankylosis, it retains the growth potential and prevents facial asymmetry on that side post-surgery. The rib cartilage, when used for nasal bridge reconstruction, should be left out of the body for 30 min to deform, prior to final carving and placement in its recipient site. This is because the inherent stress within the cartilage takes that much time to manifest which if not elapsed before placing the cartilage may cause deformation of an initially satisfactory result with time.
The incision for harvesting the rib graft is placed such that it is inconspicuous after surgery. It is placed in the inframammary crease. After careful dissection of the skin, subcutaneous tissue and the anterior chest wall muscles, the periosteum of the ribs are reached. The periosteum is stripped carefully from the rib bone on all aspects except on the posterior aspect to prevent any perforation of the pleural cavity that covers the lungs. After careful dissection, the periosteum on the posterior aspect is also released. The rib graft is harvested now and then an examination is made of the deep periosteal surface to see whether there are any pleural tears. Water is then placed in the wound and the anesthetist is asked to exert positive pressure ventilation to see whether there is any bubbling in the wound which indicates a pleural tear. If there is an air leak it is wise to use a temporary chest drain inserted through a separate stab incision in the skin. The muscle, periosteum, subcutaneous layer and skin are closed in separate layers with resorbable sutures.
This kind of surgery is available @ Richardsons Dental And Craniofacial Hospital By our Surgeon Dr. Sunil Richardson, a renowned Maxillofacial Surgeon.